Forehead Thermometer Accuracy: Debunking Myths About Forehead Fever Scanners
During the global pandemic of 2020, there was considerable media coverage about “fever scanners” and other devices designed to measure skin surface temperature. Even Dr. Fauci, NIH Director, weighed in on the subject in an interview with the chief of medicine at Walter Reed Army Medical Center (August 13, 2020).

Forehead scanners are “notoriously inaccurate,” according to Dr. Fauci. He referenced his local weather of 90+ degrees and how that affects skin temperature. “So I went into the White House the other day, my temperature was 103 until I took it in the air-conditioned car, and it was 97.4.”
While this article focuses on body temperature screening, the lessons on accurate emissivity targeting, calibration, and spatial resolution are foundational for all thermal imaging applications – from furnace monitoring in steel mills to predictive maintenance in manufacturing.
The accuracy and effectiveness of temperature screening depend on many factors. Let’s address the measurement device and screening methods.
As Dr. Fauci mentioned, such substantial variance in human body surface temperature measurements can be expected when utilizing a non-contact handheld single-spot IR Thermometer (a.k.a. forehead scanner) as it is aimed at a person’s forehead or temple. These devices detect surface temperature, which may not reflect the body’s core temperature, which is crucial for accurate fever detection. In contrast, a digital thermometer is a reliable tool for measuring body temperature, offering accuracy and versatility in various temperature reading methods, such as oral, rectal, and armpit. That surface temperature is affected by ambient temperature, and forehead readings are inconsistent from person to person, according to the National Library of Medicine. Testing has shown that the forehead varies from 2°F to 10°F lower than the body’s core temperature.

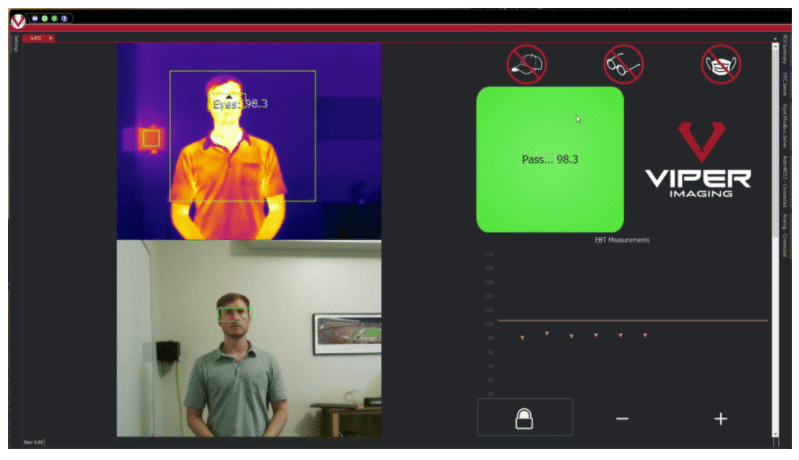
Note the image example, where the tear duct region is being measured and getting a reading of temperatures of 98.3°F (36.8°C). At the same time, a reading on the forehead measures 90.6°F (32.6°C) – a difference of 7.7 °F.
Temperature readings through non-contact means are not straightforward.
Body Temperature vs. Skin Temperature
Since forehead scanners do not accurately reflect a person’s core temperature, thermal imaging cameras answer the need for a non-contact method of measuring core temperature. This is achieved by measuring a person’s tear ducts to measure body temperature accurately. According to IEC report 80601-2-59, “evidence indicates that the region medially adjacent to the inner canthi is the preferred site for fever screening due to the stability of that measurement site. This is because the region is directly over the internal carotid artery.” The goal of measuring body temperature accurately is achieved by analyzing temperature readings from the inner canthi.
Understanding normal temperature is crucial in determining health conditions, particularly fever. The average normal body temperature is 98.6°F (37°C), but it can vary depending on factors such as age, activity, and the time of day, emphasizing its importance in accurate medical assessments.
Thermal imaging cameras measure an object’s radiated infrared energy and mathematically convert that to a temperature based on the object’s radiance. Each pixel on the camera has a calibrated temperature reading, emphasizing the importance of accurate temperature readings for effective fever screening. This is why the FDA advises adherence to the requirements set forth by the ISO and IEC for thermographic screening (FDA: Thermal Imaging Systems and COVID-19).
The Viper Elevated Body Temperature (EBT) Detection System automatically seeks out and measures a small area adjacent to the inner canthi as prescribed and recommended by the FDA, per the ISO and IEC. Viper EBT software then characterizes the inner canthi surface area temperature into a high-quality representation of the human body core temperature. Low-cost handheld IR thermometers do not have the required optical resolution to measure the small area of the inner canthi. They cannot report accurate temperature measurements on a repeatable basis, person to person, day after day, month after month. The Viper EBT System is designed and proven to produce reliable measurements over extended periods.
Why use ambient temperature screening at all?
As a means of helping to prevent the spread of illness (such as COVID-19), thermal imaging systems serve as a pre-screening device. They identify elevated body temperature (EBT), which could indicate a fever (one of the symptoms of a viral infection). In addition to thermal imaging systems, infrared thermometers, and non-contact infrared thermometers are commonly used for quick screenings in various settings; mercury thermometers offer a rapid and non-invasive way to measure body temperature. While thermal imaging systems are not medical devices and do not replace conventional medical testing, they can be used to give an early indication when appropriately used. According to the CDC, 85% of those admitted to the hospital in 2020 with confirmed cases of Coronavirus had fever symptoms.
Along with appropriate follow-up (i.e., referral to a medical professional for clinical diagnosis), thermal screening “can be useful to separate potentially infectious individuals from others.” The report cites examples of locations for use:
- Medical facilities
- Critical infrastructure facilities
- Workplaces
- Schools
- Government buildings
- Police and fire stations
- Communal locations
- Public transportation
In a 5/13/2020 discussion of thermal imaging systems, the FDA suggests consideration of temperature screening for “airports, workplaces, grocery stores, concert venues,” and “other areas where you are trying to screen large groups” as “part of a larger approach to risk management.”
Case Study: Viper Helps Keep Business Rolling
Poplar Creek Bowl is an entertainment complex including 32 bowling lanes, a sports bar, restaurant, and banquet facility. As was the case across most of the US due to the pandemic, the Illinois governor ordered a business shutdown in March of 2020. Two weeks turned into two months, so the business owner diligently explored ways to safely reopen.
How is the Viper EBT System more accurate than other non-contact infrared thermometers on the market?
First, we understand the application and how to make the measurement correctly.
- Setup and operations guides for Viper EBT systems align with best practices set forth by the FDA and IEC.
- We know that, by following these best practices, the tear ducts (inner canthi) are the reliable area on the face to obtain core body temperature. For infants under three months and young children up to age three, rectal temperatures are crucial for obtaining the most accurate readings.
- Screen one person at a time.
- We understand the requirement for cameras to have a small spot size and utilize the correct optics and distance measurement.
- We utilize Calibrated Reference Emitters in the scene’s field of view (FOV). That temperature is fed back into the software and compared to what the thermal imaging camera reads. If there is any error on the camera, the EBT system constantly corrects that within the software by recalibrating the camera so that it reads correctly based on a known source. Additionally, ensuring the thermometer is kept steady and the subject remains still during the measurement is crucial for accurate readings, mirroring the precision required in using forehead thermometers effectively.
By using these methods, the Viper EBT system can achieve better than 0.5°F accuracy.
Is the Viper EBT System Automated?
Yes. ViperVision software has integrated facial recognition to sense subjects in the screening area and then measure their temperature. This process typically takes 1 to 3 seconds. If the temperature during the measurement is below a certain threshold, the person will get an on-screen Pass result (or green box). If their temperature exceeds the set threshold, they will get a Fail result (red box on screen).
For infants, particularly those under 3 months of age, it is crucial to use rectal temperature for accurate readings when determining fever.
Can the Viper system be tied into Access Control?
Yes. Since we use different communication protocols (Digital IO, OPC, Modbus, Ethernet IP), we can communicate with external devices (both input and output). ViperVision software also allows the system to be monitored remotely.
A practical part of efforts to minimize exposure and prevent the spread
The primary objective of thermal screening is to measure temperature to identify individuals with elevated body temperature. As stated, thermal screening cannot diagnose any viral infection. Still, it has been recognized by the FDA and ISO as a practical part of efforts to minimize exposure to infected individuals and help prevent the spread. Monitoring a child’s temperature is crucial as it is a key indicator of illness. If you or your organization is considering implementing thermal screening, do your due diligence. Research the vendor and the equipment used in the system. We hope this post has helped you know what to ask.
While the Viper EBT System exemplifies precision in human temperature screening, the technology and expertise behind it extend far beyond healthcare. The same infrared principles—accurate calibration, spot-size control, emissivity management, and reliable environmental compensation—are critical to industrial process monitoring. Viper Imaging applies this expertise daily in demanding applications such as flare stack monitoring, steel ladle refractory monitoring, gas leak detection, and predictive maintenance for heavy equipment. If you’re exploring how thermal imaging can reduce downtime, improve safety, or enhance operational visibility in your facility, we invite you to download our company overview brochure or explore industrial solutions.
Do you have questions for us?
Sources:
-
IEC (International Electrotechnical Commission) 80601-2-59: Medical Electrical Equipment – Particular requirements for the basic safety and essential performance of screening thermographs for human febrile temperature screening
-
ISO (International Organization for Standardization) technical report 13154: Medical Electrical Equipment – Deployment, implementation and operational guidelines for identifying febrile humans using a screening thermograph
